What Causes Tooth Decay?
Tooth decay is caused by the presence of harmful bacteria, primarily Streptococcus mutans, in our mouths that covert the sugars we consume into acids that wear away at our enamel.
These acids initiate a process known as demineralization in which they gradually erode away at the protective covering of our teeth. This erosion is the main characteristic of tooth decay and, if left unchecked, can lead to the formation of cavities.
Further, our diets play a big role here - consuming sugary and acidic foods and drinks provides a food source for Streptococcus mutans, allowing them to continue causing acid byproducts.
To prevent, stop, and reverse tooth decay, we can use tools like remineralizing toothpaste and expandable dental floss which allow us to remove bacteria and plaque while strengthening our enamel.
In this article, I'll explain everything you need to know about what causes tooth decay and how we can prevent it from progressing into full blown dental caries.
So, what is tooth decay?

Tooth decay, a progressive stage of enamel demineralization, is a common dental condition characterized by the gradual degradation of the tooth structure.
The tooth decay process occurs when acids produced by the bad bacteria in our mouth, primarily Streptococcus mutans, interact with sugary foods and drinks from our diet. This interaction leads to the formation of acids that attack the tooth's hard outer layer, which we call enamel.
When the acid produced attacks our enamel, this initiates a process that we call demineralization. Over time, demineralization leads to the initial stage of cavity formation which can result in the development of small openings in our enamel. The openings get progressively larger and eventually penetrate deeper into the tooth, causing symptoms like sensitivity and discomfort.
Eventually, these untreated cavities can no longer be remineralized and must be treated by a dentist through treatments like dental fillings.
To reverse or prevent tooth decay, we use tools like nano hydroxyapatite toothpaste to stimulate a process called remineralization (aka the opposite of demineralization).
The 5 Stages of Tooth Decay

Tooth decay, also known as dental caries or cavities, typically progresses through five stages:
-
Demineralization: This is the initial stage of early tooth decay, characterized by the loss of minerals from the tooth enamel due to acid attacks from bacteria. The enamel is softer, but it is still possible to remineralize and reverse tooth decay.
-
Enamel Decay: In this stage, the demineralization progresses, and the enamel begins to break down. Small cavities or lesions may form on the surface of the tooth. At this point, professional dental treatment may be necessary to address the damage, although the use of nano hydroxyapatite or fluoride toothpaste may also help.
-
Dentin Decay: If left untreated, decay can penetrate the enamel and reach the dentin, the softer layer beneath the enamel. Dentin decay progresses more rapidly than enamel decay and may lead to increased tooth sensitivity and discomfort.
-
Pulp Involvement: In this stage, decay advances through the dentin and reaches the pulp, which contains nerves and blood vessels. This often results in severe pain and requires immediate dental intervention, typically in the form of a root canal treatment.
-
Abscess Formation: If decay continues to progress without treatment, it can lead to the formation of an abscess, a painful pus-filled infection at the tooth's root. Abscesses can cause severe tooth pain, swelling, and systemic health issues and require prompt dental attention.
Understandably, early intervention is key to preventing the progression of decay and avoiding more extensive dental problems. In the event tooth decay advances to later stages, be sure to seek out a dentist for professional tooth decay treatment.
Tooth Decay vs. Cavities

Tooth decay and cavities are interconnected terms used to describe different aspects of the same condition.
First, tooth decay is the broader concept, representing the gradual process of damage to tooth enamel. This process occurs when acids produced by oral bacteria interact with sugars and fermentable carbohydrates in our diets.
As these acids attack the enamel, it undergoes demineralization and gradually loses its mineral content. Tooth decay is a continuous process that can progress over time if preventive measures are not taken.
Cavities, on the other hand, are the physical manifestations of advanced tooth decay. They are the actual holes or openings that form in the enamel when demineralization progresses unchecked.
Cavities are permanent structural defects in the tooth and require dental intervention to remove the damaged portion and restore the tooth's integrity.
In essence, tooth decay is the underlying process that leads to the development of cavities, and preventive measures aim to stop or reverse tooth decay in its early stages to prevent the formation of these cavities.
Who is most at risk for tooth decay?

Several factors can increase the risk of tooth decay, and individuals with specific characteristics or habits are more susceptible.
Let's walk through some of these groups together.
Children and Adolescents
Younger individuals often have less established oral hygiene routines and may not fully grasp the importance of regular brushing and flossing.
Additionally, diets during childhood and adolescence tend to be higher in sugary and acidic foods and beverages, which can contribute to tooth decay. In fact, baby bottle tooth decay is a common condition caused by the sugars in milk.
You may hear that dental sealants and fluoride treatments are often recommended for children to help protect their developing teeth.
Seniors
Older adults may face an increased risk of tooth decay due to several factors. Many seniors take medications that can lead to dry mouth (also known as xerostomia), which reduces saliva production.
Saliva helps neutralize acids and remineralize enamel. Seniors may also have receding gums, exposing the tooth roots, which are more susceptible to decay.
Individuals with Poor Oral Hygiene Habits
Those who do not maintain proper oral hygiene habits, such as brushing with nano hydroxyapatite at least twice daily and flossing with expandable floss, leave their teeth vulnerable to plaque buildup and decay-causing bacteria.
Inadequate oral care can result in the accumulation of harmful substances on the teeth, increasing the risk of decayed tooth tissue, cavities, and gum disease.
Frequent Snackers
People who frequently consume snacks and sugary or acidic beverages between meals subject their chewing surfaces to prolonged acid attacks. These acids can erode enamel and provide a favorable environment for bacteria to thrive.
Therefore, limiting between-meal snacking and opting for healthier snack choices can help reduce this risk.
Individuals with High Sugar Diets
Diets rich in sugary and carbohydrate-heavy foods provide a constant source of nourishment for harmful oral bacteria. These bacteria produce acids that can demineralize tooth enamel, leading to cavities.
Therefore, reducing the consumption of sugary foods and beverages and maintaining a balanced diet can mitigate this risk.
What causes tooth decay?

Demineralization and tooth decay are primarily caused by the interaction of acids with tooth enamel. These can be dietary acids or simply acids produced by the bad bacteria in our mouth.
Let's walk through some of the main causes of demineralization.
Bad Bacteria & Plaque
Dental plaque is a thin, sticky film that naturally forms on our teeth. It consists of bacteria colonies that feed on sugars and carbohydrates from the foods we consume.
As they metabolize these sugars, they produce acids as byproducts. These acids can gradually erode the minerals, primarily calcium and phosphate, from our teeth which leads to demineralization.
Regular brushing and flossing help remove dental plaque, reducing the presence of acid-producing bacteria and their harmful effects on enamel.
Dietary Acids
Consuming acidic foods and beverages can directly introduce acids into our mouths, disrupting our oral pH.
For example, citrus fruits, carbonated sodas, and fruit juices are naturally acidic. When these acidic substances come into contact with tooth enamel, they can weaken the enamel's mineral structure, making it more susceptible to demineralization.
Limiting the intake of acidic foods and practicing good oral hygiene can help mitigate the impact of these dietary acids on teeth.
Poor Oral Hygiene
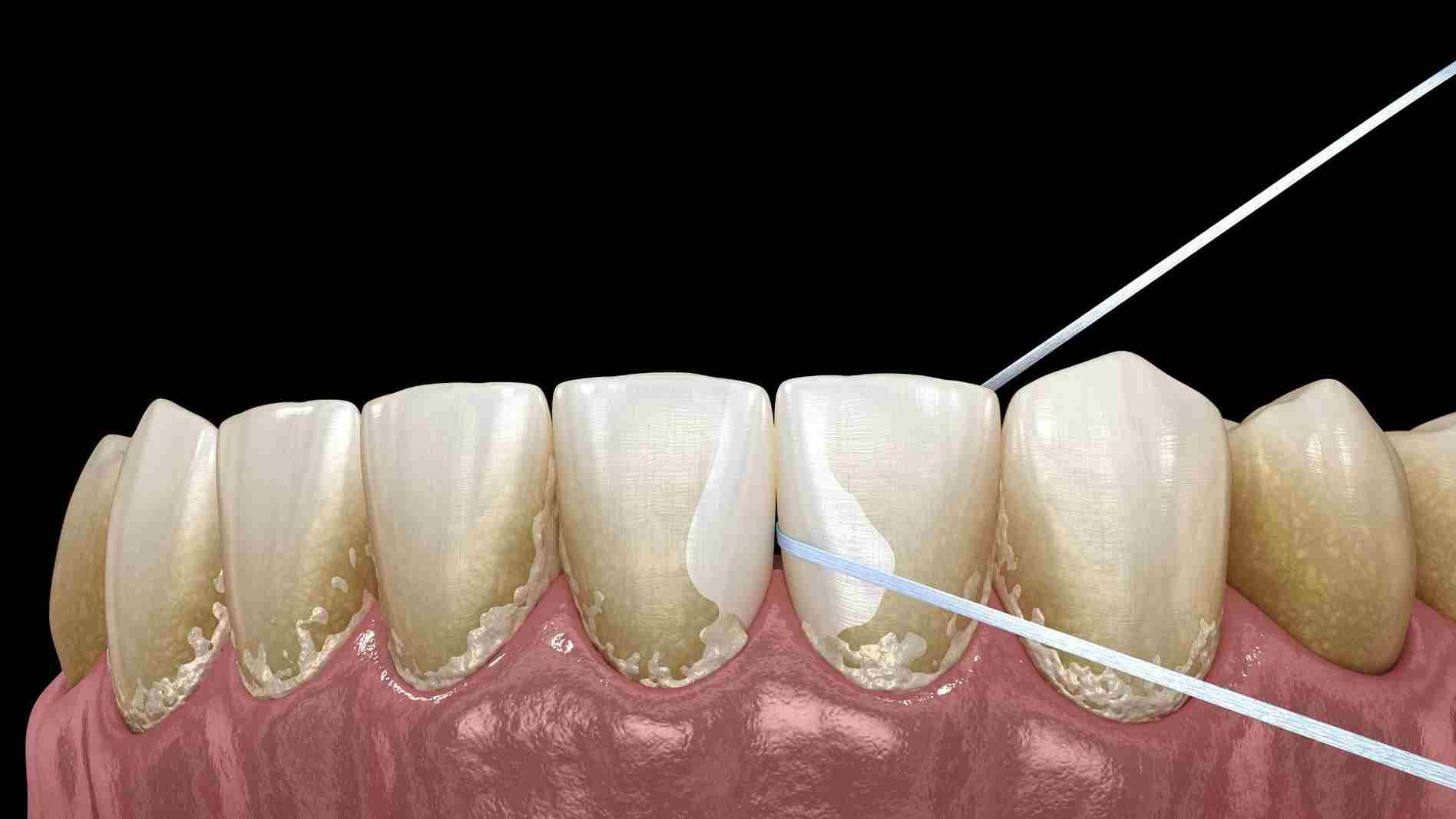
Inadequate oral hygiene practices, such as infrequent or insufficient brushing and flossing, can lead to dental plaque accumulating on tooth surfaces.
When plaque is not regularly removed, it provides a breeding ground for acid-producing bacteria. These bacteria thrive in the plaque and continuously generate acids as they metabolize sugars.
The prolonged exposure of teeth to these acids can result in demineralization, making regular and thorough oral care essential for preventing enamel damage.
Dry Mouth
Saliva is known for its ability to neutralize acids and support the remineralization of enamel. It's an essential component of your oral microbiome.
However, conditions that reduce salivary flow, such as certain medications, medical conditions, or dehydration, can leave the mouth dry. In a dry mouth environment, acids are not effectively neutralized, and the protective effects of saliva are compromised.
This can lead to an increased risk of enamel demineralization and tooth decay, making it essential for individuals with dry mouth to manage this condition effectively.
To combat dry mouth, certain toothpastes and chewing gums contain xylitol, a compound that has been proven to promote saliva production and normalize oral pH.
Acid Reflux
Conditions like acid reflux (gastroesophageal reflux disease or GERD) or frequent vomiting expose teeth to stomach acids, which are highly acidic and corrosive.
When these strong acids come into contact with tooth enamel, they can rapidly erode the minerals from the enamel surface, leading to demineralization.
Individuals with these conditions are at an elevated risk of enamel damage, and managing acid reflux or vomiting episodes is crucial to protect dental health.
Signs of a Cavity

Signs and symptoms of a cavity can vary depending on the stage and severity of the decay Let's walk through some of them now.
Toothache
A toothache is often one of the most common and noticeable signs of a cavity. It typically presents as a persistent, dull, or sharp pain in the affected tooth or the surrounding area.
You may experience worsening pain when eating or drinking hot, cold, sweet, or acidic foods. This occurs because the cavity has reached the inner layers of the tooth, where nerve endings are located.
Tooth Sensitivity
Increased tooth sensitivity can occur when the enamel has eroded due to the cavity. As mentioned above, you may experience a sharp, sudden pain or discomfort when consuming hot, cold, sweet, or acidic foods and beverages.
The exposed dentin, a softer layer beneath the enamel, is more sensitive to temperature and stimuli.
Visible Holes or Pits
In more advanced stages of decay, cavities can create visible holes, pits, or depressions on the tooth's surface. These can vary in size and appearance, but they are often a clear indication of tooth decay. You'll probably need a dentist's help to see them though, especially if they're present in your molars!
Staining or Discoloration
Cavities can cause discoloration on the tooth's surface. The affected area may appear white, brown, or black, depending on the severity and the extent of bacterial activity. This staining is a visual indicator of enamel breakdown and decay.
Pain When Biting
If you experience pain or discomfort when biting down on food, it may be a sign of a cavity. The pressure exerted during biting can aggravate the nerve endings within the tooth, leading to pain or a sharp sensation.
Pus Around Teeth
In advanced cases of tooth decay, especially when left untreated, an abscess may form at the root of the tooth. An abscess can cause the accumulation of pus, leading to swelling and the appearance of a pimple-like bump on the gums near the affected tooth.
This is a serious condition that requires immediate dental attention.
Bad Breath
The presence of a cavity can result in persistent bad breath or an unpleasant taste in the mouth. Bacteria in the decayed area produce byproducts that can contribute to foul odors and an unpleasant taste.
Complications of Cavities

Cavities (tooth decay) can lead to several complications if left untreated. Some of the common complications and associated issues include:
-
toothache
-
infection
-
abscess formation
-
tooth fracture
-
tooth loss
-
and gum disease
To avoid these complications, it's crucial to prevent tooth decay in the first place by practicing good oral hygiene by brushing with nano hydroxyapatite toothpaste and visiting the dentist regularly.
Wait, are cavities contagious?
Cavities themselves are not contagious, but experts suggest the bacteria responsible for causing tooth decay can be transmitted from one person to another through activities that involve the exchange of saliva.
The primary culprits are Streptococcus mutans and other cavity-causing bacteria; when people with active cavities or a high bacterial load in their oral microbiome engage in activities like kissing, there is a potential risk of passing these bacteria to others.
However, it's important to note that not everyone who comes into contact with these bacteria will develop cavities. As we discussed earlier, the development of cavities depends on a combination of factors, including an individual's oral hygiene practices, diet, and genetic predisposition in addition to the presence of cavity-causing bacteria.
How to Prevent and Treat Tooth Decay

To prevent, treatment, and remineralize tooth decay, we can take measures such as:
-
brushing twice daily with nano hydroxyapatite toothpaste
-
flossing with expandable floss at least three times per week
-
using a tongue scraper nightly to get rid of harmful bacteria
-
and eating a healthy diet low in acidic or sugar foods.
Specifically, brushing your teeth at least twice a day for two minutes each with nano hydroxyapatite and a soft-bristled toothbrush will help remove plaque and disrupt the growth of harmful bacteria.
In fact, nano hydroxyapatite is a biomimetic agent that mimics the natural composition of our permanent teeth and supports remineralization. Basically, nano hydroxyapatite toothpaste deposits calcium and phosphate ions back into enamel which strengthens it and makes it more resistant to demineralization.
Further, we do have some evidence that nano hydroxyapatite may prevent cavities, although it is not an approved tool by the FDA to do so.
Of course, visiting the dentist regularly and limiting sugary and acidic foods are also essential steps to take to promote good oral health. Instead, consider adding natural probiotics to your diet such as fermented foods or calcium rich foods to support your overall health.
Summary: Tooth Decay Causes

Tooth decay, the initial stage of dental caries, is primarily caused by a combination of harmful bacteria, diets high in sugars, and the lack of remineralization.
First, harmful bacteria in your mouth, particularly Streptococcus mutans, feed on the sugars from the foods we consume, producing acids as byproducts. These acids eat away at the protective coating on our teeth over time which leads to tooth decay and the formation of cavities.
Thankfully, we have tools like remineralizing toothpaste with nano hydroxyapatite and expandable floss which can help stop and prevent tooth decay.
Frequently Asked Questions
What is the main cause of tooth decay?
The primary cause of tooth decay, also known as dental caries or cavities, is the presence of harmful bacteria in the mouth, primarily Streptococcus mutans. These bacteria interact with dietary sugars and fermentable carbohydrates from food and beverages, leading to the production of acids as byproducts. These acids can erode the protective enamel of the teeth over time, initiating the process of tooth decay.
How can I stop my teeth from decaying?
To prevent tooth decay, it's essential to brush your teeth with nano hydroxyapatite toothpaste for two minutes twice a day and to floss daily to remove plaque from between your teeth and along the gum line. Further, you'll want to limit sugary and acidic foods and beverages in your diet and minimize snacking throughout the day. Of course, you should visit your dentist at least once per year for a cleaning and a checkup.
Can tooth decay be cured?
Yes, tooth decay can be effectively treated certain procedures depending on the extent of it. Early stages of tooth decay may be remineralized by brushing with nano hydroxyapatite toothpaste twice daily. If the decay has progressed, dentists may use dental fillings to remove the decayed portion and fill the cavity. Further, if the decay has reached the inner pulp and caused infection, you may need a root canal to remove the infected tissue. In cases of severe decay, your dentist may consider tooth extraction. Of course, preventative measures like brushing with remineralizing toothpaste and maintaining a healthy diet are essential to prevent future tooth decay.
Why are my teeth so decayed?
The reasons for experiencing significant tooth decay can vary from person to person but often result from a combination of factors. Poor oral hygiene practices, such as infrequent brushing and flossing, can allow plaque buildup which provides a breeding ground for cavity-causing bacteria. Additionally, a diet high in sugary and acidic foods and beverages can contribute to decay. Genetics can also play a role, as some individuals may be more prone to cavities due to their genetic makeup. If you've been experiencing extensive tooth decay, it's crucial to consult with a dentist to assess your specific situation.
What does a Stage 2 cavity look like?
A stage 2 cavity, also known as moderate enamel decay, typically appears as a noticeable lesion or discolored spot on the tooth's surface. It often takes on a white, brown, or dark appearance, indicating demineralization of the enamel. At this stage, the enamel may not have broken down entirely, but the damage is more apparent than in early stages. When inspected by a dentist, it may require dental imaging, such as X-rays, to assess the extent of the decay beneath the enamel.